The Opportunity Ahead: A Conversation with Wells Fargo Executives Mark Cotsakis and Lori Coombs
If the number of face-to-face meetings at NIC’s recent conference in Houston are any indication of activity, then the future of senior housing looks bright. Take, for example, Wells Fargo Managing Directors Lori Coombs and Mark Cotsakis. They had a combined total of about 55 meetings over the course of the 2-1/2-day conference. They came away with a real sense of energy and optimism as the industry looks past the pandemic, incorporates lessons learned and strategizes for what’s ahead.
the number of face-to-face meetings at NIC’s recent conference in Houston are any indication of activity, then the future of senior housing looks bright. Take, for example, Wells Fargo Managing Directors Lori Coombs and Mark Cotsakis. They had a combined total of about 55 meetings over the course of the 2-1/2-day conference. They came away with a real sense of energy and optimism as the industry looks past the pandemic, incorporates lessons learned and strategizes for what’s ahead.
NIC Chief Economist Beth Mace caught up with Coombs and Cotsakis after the conference to get their insights on the current lending environment and the future of the sector. What follows is a recap of their conversation.
Mace: Can you tell us about your roles at Wells Fargo?
Cotsakis: I’ve been in commercial real estate banking for 34 years. I started the senior housing group at Wells Fargo eight years ago and currently have 20 people on my team. About 85% of our business is senior housing, and 15% is medical office and life sciences. We specialize in balance sheet-based acquisition, re-position, renovation, and construction financing with a focus on private-pay rental independent living, assisted living, and memory care facilities. We provide national coverage with office hubs in both Charlotte run by Sarah Peerson and Washington, D.C. run by Erin Peart. Anne Hampton leads our underwriting team. The bank has several other groups that touch senior housing. We have a healthcare banking group that handles business with REITs and publicly traded healthcare companies. Our tax-exempt bond group works mainly with nonprofit providers.
Coombs: I have been in commercial real estate for over 20 years and oversee the agency lending side with Fannie Mae and Freddie Mac. Cathy Pharis covers HUD lending. We have 15 executives across the country. We started to focus more on senior housing in 2014 as the agencies developed specialized needs related to the seniors’ market. We were one of Freddie Mac’s top lenders three years in a row from 2018 to 2020 due to funding several large pools.
Mace: For senior housing, what is the size of Wells Fargo’s portfolio of loans? Is it expanding? How about skilled nursing?
Cotsakis: We focus on for-profit rental independent living, assisted living, and memory care. However, we specifically decided to stay away from financing skilled nursing. We felt we could be most impactful in the middle acuity segment of the market. We have a portfolio of $3.5 billion of commitments and $2.5 billion of funded positions on the balance sheet. The $1 billion difference is made up of construction loans that we have originated but not funded. Our portfolio has been expanding, with 25% growth in 2021. This loan growth was fueled by loan run-off slowing down due to market illiquidity during the pandemic despite new loan origination being moderately down relative to pre-pandemic levels.
Coombs: Our senior housing agency portfolio totals $2.6 billion. HUD offers some opportunities for skilled nursing, but our team predominately focuses on stabilized for profit rental independent living, assisted living, and memory care. Fannie Mae and Freddie Mac are cash flow lenders, and, while we have not seen many opportunities there recently, we are looking to grow the portfolio over the next couple years as census increases.
Mace: How did the pandemic affect your lending volumes? Did you look at borrowers differently? How did you underwrite loans during the pandemic?
Cotsakis: Our loan origination volume was down 25% to 30% over 2020 and 2021 in senior housing. We’ve been cautious about new loans during the pandemic. Countering that, we saw an increase in bridge and stabilization loans. As mentioned earlier, our runoff or reduction of loans on the books slowed dramatically. As we move into 2022, we expect the flow of refinance and sale activity to normalize.
Mace: Are you doing construction lending?
Cotsakis: Yes.
Mace: How does construction volume now compare to 2019?
Cotsakis: For the second half of 2021, our construction loan volume is 50% of what we did in 2019. The bigger need for borrowers is for loans that have maturities coming up. That is our focus.
Mace: Are you back to the 2019 standards of underwriting?
Cotsakis: Our loan-to-cost ratio came down 5% over the last 18 months but has moved back to a more normalized level. It’s difficult to qualify for non-recourse construction loans. Sponsor screens have intensified as we consider new business in the wake of the pandemic.
Mace: NIC’s Lending Trends Report shows a pickup in lending activity as well. On a different note, are you seeing delinquencies or foreclosures?
Cotsakis: We have had no delinquencies or foreclosures and we don’t see any on the horizon. About 80% to 90% of our loans are sponsored by private equity groups, healthcare REITs, or institutional capital. Low interest rates have helped deal with the stress.
Coombs: The agencies were offering forbearance, but we had minimal requests. We have repeat business with strong sponsors. There were some struggles, but we had limited delinquencies.
Mace: What about the emerging active adult sector? If you lend to this segment, do you underwrite it more like multifamily or senior housing?
Coombs: The agencies are still exploring active adult. Age-restricted housing is financed under the multifamily division because those properties have no commercial kitchen. It’s possible the agencies will transition age-restricted housing to the senior housing division. As far as active adult, the agencies are looking at the average age of residents and the rent premiums in relation to the age-restricted product.
Cotsakis: We have been a bigger player with rental independent living, assisted living, and memory care as our team can add more value in these more operating intensive segments. With that said, we will work with our large Commercial Real Estate team to consider active-adult but are selective on sponsorship and deals as this sector becomes more established.
Mace: Lori, you and I have been on panels discussing what NIC calls the “Forgotten Middle.” Do you provide debt to the senior housing middle-income market?
Coombs: As an agency lender, we are focused on affordability. We’re interested in expanding our exposure in the middle market; however, the opportunities have been limited. We financed an independent living project with small individual buildings with 15 rooms around a central core kitchen and gathering area. We’d like to see more opportunities in the middle market space.
Cotsakis: We have deals closing on two independent properties with rents in the high $2,000s to low $3,000s range. But it’s hard to get rents like that in projects that include assisted living and memory care because of the growth of both construction and care costs. Shared rooms can bring costs down, but COVID works against that. What has helped is the rising stock market and appreciation of housing prices which gives people more assets that they can use for senior housing.
Mace: What do you look for in a good sponsor?
Coombs: We look for sponsors with experience. We want them to have weathered different markets and cycles. We want to understand how they reacted when they were presented with challenges. What processes and procedures did they put in place? Over the last year, how did they keep residents safe? What are they doing to retain staff? How is the community positioned in the marketplace?
Cotsakis: We start with the sponsor and look at their track record of success. We look at the location and scope of the proposed project. A sponsor that has only done assisted living and is proposing a memory care project in a state where it has never operated is a red flag. We expect the capital sponsor to exhibit the financial wherewithal to deal with unforeseen stress like we saw in the pandemic. About 80% to 90% of what we finance has a strong capital partner. And finally, we expect our sponsors to have integrity, to be transparent with information and to have a relationship orientation. We need all three of these elements for long-term success. If the sponsor treats us like a vendor instead of a financing partner, the relationship won’t last.
Mace: The collateral for your loans is the real estate. Do you make loans to the operations of the business as well?
Cotsakis: We finance the real estate. We offer some banking services such as a purchasing card program, treasury management, and bank deposit accounts. As it relates to capital needs, a lot of operators under stress from COVID have a line of credit with their private equity or institutional capital partner. Those capital sources along with government subsidies have provided a lifeline to operators. Big operators with long-term management contracts and sustainable cash flow can get bank lines of credit. Moderately-sized operators can turn to a community bank or investors to help finance operations.
Mace: What are the opportunities as well as the challenges you see for the senior housing and care sector? In both the near term and the long-term?
Cotsakis: Regarding opportunities, we feel the number one tail wind is that we are finally almost at the front end of the 80-plus demographic surge, something the industry has been anticipating for 20 years. That’s huge. We’re seeing rent growth. With the stock market at an all-time high and the appreciation in housing prices, rent growth is being accepted. Social Security beneficiaries will get a 5.9% increase in their monthly checks in 2022. With wage and staff pressures, adult children are aware that they are going to have to pay more to provide good care for their parents. We’ve heard of 5% to 10% rent increases across the board. The quality of the product and service in the industry is much more consistent and appealing than it was 20 to 30 years ago. New infill locations will be a good opportunity. The challenges are wage inflation, COVID-related expenses, and the occupancy recovery. There will be moderate term rent concessions for those properties with lower occupancy. For buildings at 70% to 80% occupancy, front-loaded concessions might be limited to the elimination of the community fee, or to the third month rent free.
Coombs: There’s a lot of optimism out there. Rent increases are offsetting some of the wage pressures. We are hearing about much more activity in the market. Those who have been on sidelines are now saying they’re ready to transact again. Stakeholders are getting more optimistic.
Mace: You both attended the NIC Fall Conference this year, what were your key takeaways?
Cotsakis: I’ve worked 34 years in all real estate sectors, and senior housing has the nicest people I’ve met. It was great to meet face-to-face again. I had about 25 meetings, and what I heard were concerns about wage pressure, staffing, how to limit agency staffing, and COVID fatigue. Market wise, there are pockets in the Midwest, Texas, the Northeast, and the Southeast that will recover more slowly and see more concessionary pressures. Leasing was robust last spring and summer, but the recovery has been more muted this fall. COVID is still out there. We see a movement towards a normalized level of activity with an acknowledgement that it will take a few years to dig out of this hole. Finally, considering the high impact of COVID on the sector, I was struck by how many big private equity investors are attracted to the industry because of the disruption. I expect more large portfolio platform sales activity over next few years based on the big players looking to get into the market because this is their opportunity.
Coombs: I had about 30 meetings at the NIC Conference. It was busy and great to be back together. Everyone is looking at this period as an opportunity. But it will take awhile to get back to pre-COVID levels of activity; though we are seeing a more normalized environment for lending and transactions.
Mace: Any other thoughts you’d like to share?
Cotsakis: While COVID was a disruption for the industry, one byproduct was that it put a reality check on new competitors and helped to reduce new supply. It’s really good to have that mid-cycle correction. When we do hit a real estate downturn, it will help that we don’t have a lot of participants who don’t understand the industry because their operations have been rising with the tide. It’s not bad that we had a little stress. It puts pressure on those who are not as good as they needed to be to survive in this industry.
The Case for Senior Living Investments
The following is an excerpt from introductory comments provided during the 2021 NIC Fall Conference by Kurt Read, Managing Director, RSF Partners, and Chair, NIC Board of Directors.
 As an investor in this industry over the last 30 years, I think a moment of disruption like the pandemic is the perfect time to remake the case for investing in our industry. So here it goes in rapid fire NIC speed-dating style.
As an investor in this industry over the last 30 years, I think a moment of disruption like the pandemic is the perfect time to remake the case for investing in our industry. So here it goes in rapid fire NIC speed-dating style.
Despite the temporary disruptions caused by the pandemic, the market conditions for senior living investments are favorable due to both demographic trends and the structural characteristics of our market.
Demographic Trends
The population is aging. We are moving to serve the baby boomer generation which is we now serve. We are also living longer than ever before once we reach 65. Several of our sessions at this conference directly related to the implications of this profound change.
The relationship between the population of caregiving-aged Americans (those 45 to 64 years old) to those over 80 is changing. That ratio will decline from about seven-to-one today to four-to-one by 2030. The pandemic exacerbated caregiving challenges as labor participation rates have fallen precipitously.
Structural Characteristics
Our existing supply of properties is aging. 62% of senior living communities and 92% of SNFs are over 17 years old.
Senior living rents have limited correlation to the broader economy. Demand is inelastic as it is driven by need. Residents are insulated from fluctuations in the labor market as they are retired.
The industry is fragmented with nearly 60% of communities in the hands of operators who have fewer than 10 properties.
It is notoriously difficult to scale successfully in our industry. There are a variety of reasons why, but here are a few of my favorites:
- Local markets matter – customer demand, competition, referral patterns, land usage, and labor markets are driven locally.
- Operations are hard to scale as they are a complex mix of real estate, wellness, hospitality, and healthcare.
- Branding has limited effect – as most families only make the decision to consume our product once or twice in a lifetime.
- Regulations are often a confusing mix of state, local, and federal rules.
- And you can’t offshore personal care.
Opportunity
All of these factors and more make it hard to scale. But they create opportunity for those who are narrowly and passionately focused, well capitalized, and dedicated to the use of good data to make better decisions.
Well, what does the data show right now?
- Occupancy is rebounding and strong pent-up demand for our product is reflected in the record absorption in the third quarter.
- Supply growth is moderating
- Rent growth is positive
- Housing prices are up, and the single-family market is liquid.
All that is good! However, we are in unprecedented times, and government involvement in all facets of our lives hasn’t been this significant since probably World War II. This involvement means it is ever more important for all of us to understand the forces driving policy at both the state and federal level, as well as engage with our elected leaders around simple and clear-to-understand objectives.
Emerging Asset Class Captures Investor Interest - NIC Fall Conference Session: The Investment Market for Active Adult
Forget Bitcoin. The hot investment in senior living is the active adult segment. Positioned between multifamily and senior housing, the emerging asset class is designed for the growing cohort of aging baby boomers. They’re finally reaching the age where they might want more services while still maintaining their independence.
Investors want to get in on the ground floor, and many are expecting the active adult segment to grow quickly producing outsize returns.
Questions remain about the depth of the market and how it fits into the overall senior living investment spectrum. What are its prospects? Who are the early-stage investors? And how are their bets paying off so far?
Investors and owners detailed their experiences with active adult properties during a panel discussion at the 2021 NIC Fall Conference. The discussion was led by Aron Will, vice chairman, Debt and Structured Finance, co-head, Senior Housing at CBRE. He was joined by Zachary Crowe, managing director at The Carlyle Group, a global investment firm; Ayesha Menon, senior vice president, Wellness & Housing Development at Welltower, a real estate investment trust; and Jeff Patterson, co-founder & CEO at Sparrow Partners, a developer and operator focused on the active adult segment.
The first challenge is how to define “active adult.”
“Active adult is really a chameleon,” noted Will. The properties are like apartments in design and rent structure. But active adult resembles senior housing in its resident profile, attracting individuals in their early to mid-70s.
The projects are lifestyle and hospitality driven, often commanding rent premiums. The active adult segment, however, is not the same as independent living which is more likely to accommodate older seniors.
The panelists agreed that the active adult model can vary. Some projects provide meals and services such as housekeeping, while others don’t. “The right product depends on the customer, the demographics, psychographics, and the micro location,” said Crowe. “There’s no one right answer.” He believes the segment will become further stratified as it matures. “There will be different price points and service levels just as there are now with apartments and hotels,” he said. “We are still in the second inning of the evolution of the asset class.”
Investment Strategies Vary
Welltower imposes a framework on its senior housing investments based on the intersection of acuity and financial need. The REIT focuses mostly on the higher acuity, higher income end of the senior housing spectrum. Menon is leading the growth of lower acuity assets to complement Welltower’s higher acuity assets. She prefers middle market active adult projects for residents who have savings but are thoughtful about spending. Menon added that Welltower’s active adult assets have been very stable throughout the pandemic, though performance varies by location.
Sparrow Partners targets the active adult middle market with communities in Arizona, Florida, Nevada, Oklahoma and Texas. Monthly rents range from $1,700 to $1,900. About 60% of residents move into a community after selling a single-family home, representing most of their net worth. “Our customer is someone who has made choices and had to make choices,” said Patterson.
Recognizing an opportunity, The Carlyle Group launched an effort 10 years ago to create an investment thesis around the aging baby boomer demographic. The firm’s active adult portfolio currently includes a mix of acquisition and ground-up developments at different price points. The upscale Overture brand, for example, was created in partnership with developer Greystar. Crowe said that about 80% of residents in the higher price point properties have sold a single-family home. “Those residents have a higher net worth and a higher income,” he added.
High-end active adult properties are slower to lease than middle market properties because middle market residents are less likely to have the complications of selling a house. But Crowe noted that rental velocity mostly depends on the market, and resident expectations in the micro location. “We’re still learning every day what motivates people to move,” he said.
Some consumer trends are emerging. Residents want a quiet place where they can interact with their peers. They’re seeking a sense of community. And they expect programming tailored to their interests.
The panelists agreed that active adult residents tend to be “stickier” than traditional multifamily renters. Average length of stay in active adult properties is about five to six years.
While commercial real estate has had its winners and losers during the pandemic, active adult properties have performed fairly well, Will pointed out. Move-ins were never curtailed as they were at assisted living projects. Collections never lagged, and the sector saw rent growth.
Over the last 18 months, Sparrow Partners experienced solid collections and low resident turnover. Property leasing slowed and some restrictions were implemented on community activities based on local COVID mandates. “We came out encouraged about how we performed,” said Patterson.
At Carlyle properties, collections were over 99% across its 70 active adult assets. Rent growth was positive as well, turning in the best sector performance among its residential assets during COVID. Key to strong performance is low staffing levels. Crowe estimates staffing at about 4-8 full time equivalent workers per property, compared to about 30-40 staff members at other senior living properties. Also, free telemedicine services were offered to residents across the portfolio.
The Elephant in the Room
Age creep. Moderator Will asked if active adult properties can maintain their lifestyle vibe as residents age in place.
The answer is to backfill with younger residents, said Crowe. New properties have an average resident age of about 72. Residents stay five years and the average age plateaus at 74-77. Properties need to continue to attract younger people.
Sparrow Partners decided early on not to offer transportation or meals. That reduces costs but also encourages residents who need more help to move to another housing option. Home health services are not restricted but are not promoted either.
Active adult properties are attracting a wide swath of buyers from multifamily investors to private equity funds and REITs. “We see a number of opportunistic buyers,” said Menon.
Cap rates are running slightly below multifamily cap rates because of the stability of active adult assets during the downturn. Financing is available, though the agencies, Fannie Mae and Freddie Mac, are still exploring how to classify the asset.
Sparrow Partners finances new construction with loans from regional and community banks. The most likely lenders are the ones comfortable in the space with several active adult assets already on the books. Patterson expects lending capacity to expand as sales increase.
While the advantages of scale in senior housing have produced portfolio premiums, the panel agreed that active adult isn’t a good candidate yet. There just aren’t enough stabilized properties to aggregate.
The Path Ahead
The big lessons learned so far?
“Micro and macro location is key,” said Menon, noting that performance differences cannot be explained by other factors. “It comes down to location.”
Sparrow Partners is digging into the marketing details. “We are still trying to figure out how many units a month will rent,” said Patterson. Early projects were underwritten with a projected lease-up of 12-15 units a month. “Don’t do that,” cautioned Patterson, explaining that the project could then run into financial trouble. He thinks 6-10 units a month is a more reasonable leasing goal.
Crowe said that the operator is particularly important and must understand a product that is a little bit multifamily, senior housing and hospitality mixed together. “You need the right operator and the right sales pitch,” he said.
Data transparency will be essential to move the segment forward as an established property type, the panelists agreed. Institutional and other investors have come to expect robust data to track performance, a more difficult ask in the still developing active adult space.
Three Scenarios: Estimating the Recovery in Senior Housing
by Beth Mace, Chief Economist, and Lana Peck, Senior Principal
Most senior housing stakeholders want to know when market fundamentals will return to pre-pandemic levels and what that path will look like. While neither NIC Analytics nor NIC MAP Vision generate forecasts per se, we can provide some context from which to consider the path of recovery by market and property type. This article presents one way to look at recovery timelines by creating three scenarios of possibilities based on recent and historic demand patterns. We conclude that market and product type recovery depend upon three things: how much net demand was lost due to the pandemic, the level of construction that occurred during the pandemic, and the current development pipeline. As a result, the recovery timeline is different for independent living versus assisted living, and by metropolitan market, and could possibly occur as quickly as one or two years, or as long as seven or more.
Introduction
It was welcome relief by many to see that third quarter data from NIC MAP Vision showed an uptick in senior housing occupancy following the previous five quarters of pandemic-related weakness. The occupancy rate for senior housing increased by 1.4 percentage points to 80.1%. By majority property type, assisted living occupancy rose from its record low of 75.4% in the first and second quarters of 2021 to 76.9% in the third quarter, while independent living rose from a higher but still low rate of 81.9% to 83.2%. The occupancy rate for assisted living remained 4.9 percentage points below its pre-pandemic first quarter 2020 level of 85.0%, while independent living was well below its prior recent peak of 89.7%. The question remains on how quickly a fuller recovery will occur.
The pandemic was an incredibly difficult and challenging time for virtually all businesses in the U.S. as well as across the world. Business leaders loathe uncertainty, and the COVID-19 health crisis wins the penultimate gold medal prize for uncertainty. Unfortunately, with the uncertainty of the new Omicron variant, the COVID-19 health crisis continues to hold on to that title.
During this global health emergency, operators of senior housing properties reacted as fast as they were able and proved themselves to be reliable care givers of their stewards as well as agile, flexible, and nimble to adjust to the often-daily-changing protocols and rules being promulgated by federal, state, and local government agencies. Further, many operators of senior housing properties self-imposed moratoriums to limit the entry of new residents to prevent outside contamination to existing in-place residents.
As a result, between the second quarter of 2020 and the second quarter of 2021, these move-in restrictions contributed to the largest fall-off in the number of occupied units to ever be recorded for senior housing. Occupied units plummeted to levels last seen in mid-2017 as 42,344 senior housing units were placed back on the market across the 31 NIC MAP Primary Markets.
Three Buckets of Recovery Units
For this analysis, we will define three categories or buckets of units that will comprise the senior housing units that need to be recovered or “absorbed” on a net basis within the Primary Markets if pandemic conditions are to be reversed.
- Vacated Units
This first tranche of recovery units is comprised of 42,344 previously occupied units that were placed back on the market between first quarter of 2020 and first quarter of 2021 due to the pandemic and were not filled as they became vacant. For senior housing in the Primary Markets, this can be seen in the table below as the first row. Between the second quarter of 2020 and the second quarter of 2021, move-in restrictions contributed to the largest reduction in the number of occupied senior housing units ever recorded by NIC MAP. - New Inventory
The second tranche of units that need to be absorbed are those units that opened during the pandemic from the first quarter of 2020 to the third quarter of 2021. New inventory offers a fresh competitive set for many existing properties, thereby impacting the ability to rent stabilized units in the marketplace. As the table below shows, for senior housing in the Primary Markets, this totals 30,773 units.Notably, senior housing inventory growth slowed during the pandemic but remained relatively robust, with 3,441 units added to inventory in the third quarter alone. That said, inventory growth has generally trended down from its high point of 6,100 units in mid-2019. Growth in the stock of senior housing is likely to continue to be moderate for the next year or longer due to a pandemic-related slowdown in construction starts in the past 18 months. - Units Under Construction
In addition to those units that opened during the pandemic, there are still units that are currently under construction that will be opened in the coming two years. These development units are estimated to total 33,014 for senior housing in the Primary Markets. The number of units under construction moderated during the pandemic due to uncertainty as well as cautious lending by banks and other lenders. In fact, by the third quarter, senior housing saw the fewest units under construction since 2015.How quickly will these three buckets of unoccupied potential demand be filled? The pace of recovery by market and by property type will depend upon several factors which will be enumerated further below. Foremost among them are the degree of pent-up demand. During the pandemic, many potential new residents simply did not move into senior housing properties. At times this was due to moratoriums imposed by a government entity or by the property managers/owners themselves to limit the spread of infection. In other instances, fears of quarantine and isolation and economic insecurity kept potential new residents away. And lastly, with many adult children unable to work due to furloughs and layoffs, some family members decided to care for their aging parents themselves.Once the vaccine became available in January 2021 and as more properties “re-opened” to new residents in the second and third quarters of 2021, a flurry of move-ins occurred as this pent-up demand was released. Indeed, in the second and third quarters of 2021, there were 15,682 units absorbed on a net basis. Notably, net unit absorption reached a record high of more than 12,000 for senior housing in the third quarter of 2021 for the Primary Markets. This rapid pace of demand allowed total occupied units to move back to their year-earlier levels seen in the third quarter of 2020—a sharp improvement from where they stood in the second quarter at mid-2017 levels.
Recovery Scenarios
Considering the three buckets of recovery units, below are a few scenarios that may help you think about senior housing recovery timelines for benchmarking your own projections. The table shows the number of senior housing units put back into the marketplace as well as those that have been newly opened and those currently in development. These are the same three buckets of units for occupancy recovery that were previously defined.
- As shown in the table, for senior housing there were 42,344 units placed back on the market from the second quarter of 2020 to the first quarter of 2021 for the Primary Markets. There were also 30,773 units added to inventory from the first quarter of 2020 to the third quarter of 2021, and there are currently 33,014 units under development. Now consider that 15,682 units were absorbed during the second and third quarters of 2021, leaving 90,450 units to be absorbed. If those units were absorbed at the very rapid pace of the third quarter of 2021, this would take 7.3 quarters or 1.8 years. Hence a full recovery could occur by the third or fourth quarter of 2023.
- If, however, you believe that the third quarter pace of demand is not sustainable and a weaker, albeit still strong, pace of net absorption that mirrored that of the second and third quarters of 2021 were to occur, then aggregate units occupied could be achieved within 11.5 quarters, or 2.9 years. This suggests, a full recovery could occur by the third quarter of 2024.
- If, however, the pace of net lease-up was more in line with historic patterns of the past ten years, then it could take 30.7 or 7.7 years for full recovery. This suggests, a full recovery could occur by the third quarter of 2028.
Resulting in a wide range of recovery timelines, these three senior housing demand scenarios provide a framework that can be fine-tuned according to your views on the pace of market demand. Indeed, other demand assumptions could also be applied; perhaps using a five-year historical look back or a three-year look back. These scenarios can also be applied to property type and metropolitan markets as well using data from NIC MAP Vision.
Factors That Will Affect the Timing of a Full Recovery
In addition to factors such as varying the pace of absorption that was previously demonstrated in the recovery scenario table, there are many other factors that may speed up or slow down recovery from the pandemic:
- Pent-up demand: Will past performance predict future results? Has the pent-up demand that recently swept into properties in the second and third quarters been spent, or will absorption continue at the third quarter record-breaking pace?
- Demographics: Are the baby boomers finally on the doorstep of senior living? The growth in the age 80-plus cohort will expand rapidly before the end of the decade. Just this year, the age 80-plus cohort increased by 325,000 people. By 2025, it will increase 500,000, and by 2027—one million people. Many will have mobility limitations and chronic conditions that necessitate safe and social congregate care environments.
- Consumer confidence: Will senior housing capitalize on the value proposition of safety, security, health, wellness, and engagement? Or will there be growing interest in alternatives to senior housing? The better the value proposition of senior housing and care is accepted by prospective residents and their adult child influencers, the faster the industry will recover.
- Affordability: According to the NIC-sponsored Forgotten Middle Market Study, the middle-income cohort is a large and growing demographic with huge market potential. Will senior living remain out of reach for a significant and growing portion of the market—the middle-income resident—or will product segmentation strategies and lower cost alternatives enable more access and choice for the nation’s elders?
- Rents: One of the myriad challenges brought on by the pandemic was the pinch to operator margins, which came at a time when expenses were increasing due to growing costs to attract and maintain staffing levels, rising insurance costs and vacancies due to the pandemic. Will operators need to offer rent concessions to support occupancy, or will rents need to be increased to counter expense growth?
- Competition: Prior to the pandemic, some senior housing markets had excess supply, which resulted in increasing competition putting downward pressure on occupancy rates. However, oversupply had already begun to slow new construction in some markets, especially for assisted living. Starts are down since the beginning of the pandemic. Could the moderation in construction activity release some pressure on refilling occupancy in the short term?
- Appeal: The nation’s aging senior housing stock may not be adequate to meet the needs and desires of younger baby boomers entering retirement. Will developers have access to capital sources to construct new buildings and reposition older buildings to appeal to the lifestyles of new consumers? Will investor interest in lower acuity settings such as active adult (also known as 55-plus communities) expand the market for senior housing to younger consumers?
- Technology: At a time when all sectors of the labor market are experiencing shortages, deliberate use of time-saving and supportive care technologies may give senior housing caregivers more time to spend one-on-one with residents. Will senior living embrace supportive technologies to allow caregivers to efficiently care for residents, or will staffing and labor shortages continue to put a drag on occupancy in high acuity care settings and challenge lower acuity settings to provide services?
There will be different rates of occupancy recovery across metropolitan markets and within primary market areas. According to third quarter NIC MAP data, across the Primary Markets there is an 11-percentage point difference between the best and worst performing markets, and not every property within those markets will recover at the same pace. For example, some properties that managed to largely maintain their occupancy during the pandemic will recover faster than those that were new or still in lease-up when the move-in moratoriums started early in the pandemic and then when the pandemic drug on.
Indeed, individual market recovery timelines depend on many factors—macro economic conditions, housing market conditions, consumer preferences, local demographics including the influence of adult children, the competitive landscape, and more. Assumptions on the pace of move-ins and move-outs are also important considerations. These considerations can shape your view on the pace of demand and how quickly existing and new inventory will be leased.
To subscribe to best-in-class market analysis tools and the data that supports our recovery scenarios, schedule a meeting with a NIC MAP Vision product expert today.
Reaching Recovery
The degree to which demand bounced back in the last six months will shape the immediate response, while the amount of new inventory created in the past 18 months as well as current supply pipelines will dictate how quickly pre-pandemic “equilibrium” conditions can be achieved. Notably, even a recovery to pre-pandemic levels may not be the correct “endgame” because occupancy rates were challenged and trending lower for many markets prior to the pandemic. This was particularly the case for assisted living properties.
The necessary ingredients for a fuller recovery include an industry-wide push to grow penetration rates. NIC estimates that 11% of households over 75 years of age reside in senior housing. What’s up with the other 89%?
Labor Challenges in Skilled Nursing: An Overview
by Beth Mace, Chief Economist & Omar Zahraoui, Data Analyst
In a recent NIC Notes blog published on October 22, 2021, NIC Analytics examined which group of workers and roles are in high needs and have the largest labor shortages within skilled nursing facilities, and the impact shortages of these essential workers, defined as nursing staff and aides, have on skilled nursing facility (SNF) residents, SNF performance, and the recovery of the skilled nursing sector.
In this follow-up article, we provide context on jobs in the SNF sector, by looking at recent employment patterns as well as occupational data and wages for nursing care and other adjacent industry groups.
The labor issue is not something new as prior to the pandemic operators were faced with shortages due to record low unemployment rates (3.5% in February 2020). As the pandemic progressed in early 2020, the jobless rate shot up to 14.7% in March 2020 and has since settled back down to 4.2% in November 2021. Labor challenges are deeper than these statistics suggest, however, and have been exacerbated by a shrinking labor force. Workers have dropped out of the workforce in the so-called “Great Resignation.” Further, the labor force participation rate remains well below pre-pandemic levels at 61.8%. In the next few months, labor force participation rate will be a critical measure for the trajectory of the labor trends.
For the senior housing and care sector, the nation’s labor force participation rate for women is particularly problematic and at levels last seen in the 1980s. This can be traced to childcare responsibilities in many instances, as childcare options have become more limited since the pandemic began. One particularly challenged occupation in the skilled nursing sector during this time has been nurses, since 91% of nurses are women, many of whom may have home care responsibilities for both children and aging parents.
The uncertainty band remains wide as it pertains to when or if labor participation rates will return to pre-pandemic levels. NIC analysis showed the labor challenges started to lessen to a degree as COVID-19 cases started trending down following the vaccine rollout in early 2021. Notably, the share of skilled nursing facilities reporting staffing shortages among hands-on essential workers (nursing staff and aides) started declining amid increasing demand and occupancy rates. By July 2021, however, the surge in Delta variant cases and the recent vaccine mandates reversed some of this progress and staffing shortages among nursing staff and aides intensified. NIC’s Skilled Nursing COVID-19 Tracker shows that infections started rising again and the threat of the new Omicron variant is worrisome.
Shrinking Numbers of Workers in Skilled Nursing Sector
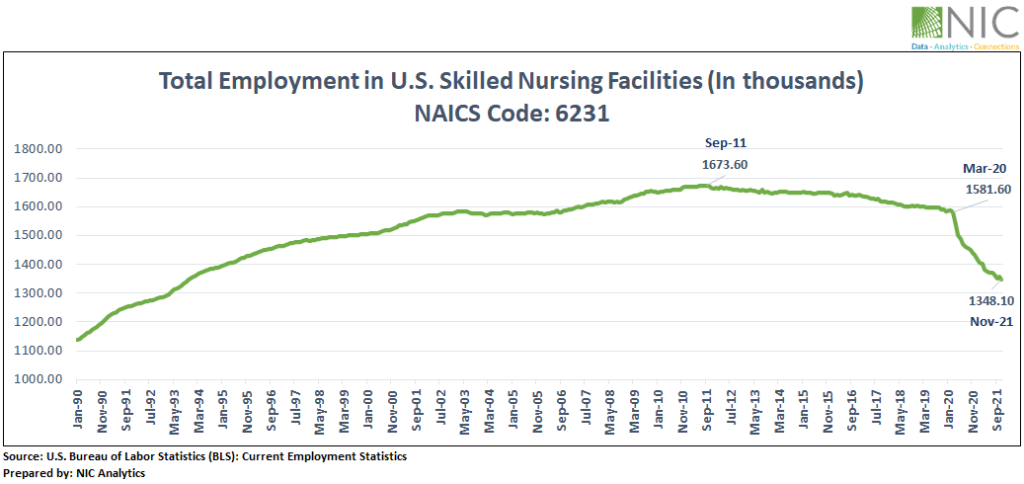
Due to the COVID pandemic and its related economic cycle, there are fewer jobs today in the SNF sector than in March 2020, the beginning of the pandemic. Indeed, according to data from the Bureau of Labor Statistics (BLS), skilled nursing facilities lost more than 233,000 jobs between the onset of the COVID-19 pandemic in March 2020 and November 2021, the equivalent to 14.8% of total workers. The November 2021 jobs report shows that the total number of workers (seasonally adjusted) within skilled nursing facilities dropped to 1.35 million (down about 8,400 workers from October 2021 levels) and is now back to September 2021 levels.
Compared with other healthcare settings, employment levels within SNFs remain far below pre-pandemic levels and are not expected yet to fully recover due to the substantial loss in demand (number of occupied beds) and the lingering low occupancy rates. Further, jobs have been on the decline in the SNF sector since 2011, with over 325,000 fewer workers employed in the sector today, or a decline equivalent to 19.4% of the workers. Some of this dropoff in workers may be explained by the sheer loss of operational beds in the sector which have fallen in the 31 NIC MAP Primary Markets, for example, from 496,000 in 2006 to 478,000 in 2021.
Where Do the Workers Work?
For context and to provide a framework for looking at labor conditions in skilled nursing and more broadly healthcare, NIC Analytics compiled 2020 data from the BLS on employment and wages by industry classification and occupational status. The main purpose of this was to benchmark labor concentration and wages in SNFs as compared to other adjacent industries and healthcare settings across all U.S. states.
Interestingly, six industries employ between 75% and 90% of the nation’s nursing staff and aides. These are: (1) skilled nursing facilities, (2) home health care facilities, (3) continuing care retirement communities and assisted living facilities for the elderly (CCRC & AL), (4) general medical and surgical hospitals, (5) individual and family services, and (6) offices of physicians. These industry groups are based on the Office of Management and Budget’s (OMB) standard industry classification codes known as the NAICS or the North America Industry Classification System.
Further, four occupations account for roughly 60% of all staff within the skilled nursing sector. These occupations are: (1) registered nurses, (2) licensed practical and licensed vocational nurses, (3) nursing assistants, and (4) home health and personal care aides. All these workers have direct and personal relationships with residents and patients. Notably, nursing assistants in SNFs totaled 527,480 workers, accounting for 34.4% of all staff within the skilled nursing sector. Similarly, licensed practical and licensed vocational nurses (LPNs and LVNs) totaled 199,760 individuals, representing 13.0% of all jobs in the SNF sector. Hence, these two occupations accounted for over 47% of all staff within the skilled nursing sector.
Further, skilled nursing facilities employed more nursing assistants, LPNs, and LVNs than any other industry and healthcare setting in 2020. Nursing assistants in SNFs account for 38.5% of the nation’s workers in this occupation, and LPNs and LVNs in SNFs represent 29.5% of the nation’s workers in this occupation.
The summary table and pie charts below provide details on employment levels and wage rates in these industry groupings as well as occupation counts. Additionally, there are other metrics created from these data points that help measure the concentration and intensity of jobs in the skilled nursing sector.
For this article, we define labor concentration as the number of employed workers in a specific occupation per 100 persons aged 80 and older, i.e., how many workers are employed per older adult. For the LPN and LVN occupation category, this equates to 5.2 LPNs and LVNs for every 100 80-year-olds, while for nursing assistants, this ratio is 10.4. By comparison, there are more workers for each older adult for registered nurses (22.8) and aides (24.5).
The concentration of workers in these four occupations vary by state. There are some states with higher ratios and some with lower ratios. For example, the highest concentration ratios for LPN and LVN occur in Louisiana (10.9), Tennessee (9.5), and Arkansas (9.2). Overall, 22 states had labor concentrations higher than the national average of 5.2. For nursing assistants, the largest labor concentration ratios were seen in North Dakota (23.9), Rhode Island (18.7), and Kansas (17.9). Thirty-seven states had labor concentrations higher than the national average of 10.4.
FTE Measurements
Alternatively, as a measure of job intensity or concentration, we have created a full-time equivalent ratio, where the ratio is defined as the total number of persons employed in the SNF industry by a specific occupation per 100 certified beds. For LPNs and LVNs, this staffing ratio is 12.1, and, for nursing assistants, it is 31.9—significantly higher than that of registered nurses (8.7).
By state, these measures vary significantly. For example, the FTE ratio per 100 certified beds for registered nurses in Texas is 4.9, 44.1% below the national level of 8.7. This is well below California, where the FTE ratio is 10.9, or 25.3% above the national level of 8.7. This is an important distinction in the context of policy discussions currently underway regarding staffing mandates. For example, if staffing mandates were to change, skilled nursing facilities in Texas may be required to implement higher minimum nursing staff-to-resident ratios, and meeting those requirements could be challenging.
Wage Rates
These last two measures provided a sense of supply versus need for specific worker occupations within the skilled nursing sector. A fuller analysis of labor conditions requires an examination of wage rates as well. At $24.62 per hour on average, LPNs and LVNs within the SNF sector were paid 2.2% above the national average of $24.08. Relative to other industry groupings, SNF workers were also paid nearly the same or better than all other healthcare setting including general medical and surgical hospitals (at $22.75 – nearly $2 less per hour than SNFs).
Wages for nursing assistant workers in SNFs were also competitive, at $14.90. Nursing assistants were paid slightly better than those in family services and home health care ($14.30) and CCRCs and assisted living properties ($14.71), but $1.28 less per hour than in general medical and surgical hospitals ($16.18).
Employment and Wage Rates in Senior Housing (CCRC and Assisted Living Properties)
Nursing assistants in CCRCs and assisted living properties employed 151,540 workers, accounting for 16.10% of all staff within these congregate settings. Similarly, LPNs and LVNs totaled 53,280 individuals, equivalent to 5.7% of all jobs in CCRCs and assisted living properties. As a comparison, these two occupations accounted for about 22% of all staff within the skilled nursing sector.
CCRCs and assisted living properties employed less nursing assistants and LPNs and LVNs compared with the skilled nursing sector in 2020. Nursing assistants in CCRCs and assisted living properties account for 11.1% of the nation’s workers in this occupation, and LPNs and LVNs represent 7.9% of the nation’s workers in this occupation.
Average hourly earnings for nursing assistants and LPNs and LVNs in CCRCs and assisted living properties were slightly lower than those of SNFs at $14.71 and $24.57, respectively, although, they were also competitive compared with the other industries and healthcare settings.
Data Takeaways
These large numbers and shares of direct care staff (LPN and LVN and nursing assistants) in SNFs and senior housing suggest that these sectors have been successful in attracting workers and competing with other industries at least prior to the pandemic in 2020 (based on the vintage of the BLS data which is date stamped April 2020). Moreover, the wage data for these two skilled nursing occupations for SNFs was competitive compared with other healthcare settings.
Looking Ahead
There are many factors that will influence labor market conditions for nursing staff and aides within both the senior housing and the skilled nursing sectors. These include broad macroeconomic market conditions, the size and growth of the labor force, staffing regulations, retention, and competitiveness. Further, while occupancy rates in both senior housing and skilled nursing have been gradually improving in recent months, the industry continues to be challenged with maintaining operating margins due to many non-occupied rooms and elevated operating expenses associated with insurance, staffing costs, and other expenses. Moreover, challenges in recruiting staff have led some operators to not accept new patients.
Provisions of the current Build Back Better legislation may further exacerbate the workforce situation in skilled nursing facilities. SNFs may be required to follow new staffing mandates, including a minimum nursing staff-to-resident ratio that would require a registered nurse (RN) to be on hand 24 hours a day, three times the current requirement of at least eight hours a day.
This article has highlighted the state of the labor market in skilled nursing and touched upon senior housing as well. Clearly there are a lot of challenges. In future commentaries, we will address other aspects of the labor market including staffing regulations, competitiveness, and retention.
NIC Analytics compiled 2020 data from the Bureau of Labor Statistics (BLS) to provide a detailed overview of occupational employment and wages by state, and pinpoint where skilled nursing facilities and senior housing properties (CCRC & assisted living properties) stood in 2020 compared with competitive landscape (i.e., other industries & healthcare settings). To request the complimentary state occupational employment and wages report, please contact us at analytics@nic.org.