An Entrepreneur Focused on Operations: A Conversation with Solera’s Adam Kaplan
 It’s no surprise that Adam Kaplan is an entrepreneur. He caught the entrepreneurial bug early in life visiting senior living communities with his father Bill Kaplan, co-founder of Senior Lifestyle. In 2016, Adam launched his own company, Solera Senior Living.
It’s no surprise that Adam Kaplan is an entrepreneur. He caught the entrepreneurial bug early in life visiting senior living communities with his father Bill Kaplan, co-founder of Senior Lifestyle. In 2016, Adam launched his own company, Solera Senior Living.
NIC Chief Economist Beth Mace recently talked with Kaplan about Solera’s brand strategy and its focus on operations, a part of the business that he says doesn’t get enough attention. What follows is a recap of their conversation.
Mace: As the founder and CEO of Solera Senior Living, what led you to start a senior living company?
Kaplan: I grew up in the industry. I would go with my dad to properties in Chicago and saw operations firsthand. I also went to ASHA’s Annual Meeting in high school and college and met industry veterans like Bill Colson and heard his incredible entrepreneurial story. I worked on the finance side at Merrill Lynch Capital and then at Senior Lifestyle for nine years in operations. I had grown up with an entrepreneurial father and wanted to pursue that path myself. I felt there was a lack of operators coming into the industry looking to innovate and saw an opportunity to change the model. I decided to build an operating company. We also have a development and investment arm.
Mace: Why did you choose the name Solera?
Kaplan: I like names with meaning. Solera is a Spanish word associated with the blending of wine of different ages. It evokes the idea that things get better with age. Solera is also a one-of-a-kind blended scotch. That resonated with me because all of our properties are unique. Not cookie cutter. They fit with the local fabric. I want to build urban infill properties in first-ring suburbs. Our buildings are places that you want to go regardless of age, whether you’re a resident, family member, employee, or service provider.
Mace: What distinguishes Solera from other senior living companies?
Kaplan: We are geographically agnostic. Most operators focus first on building scale in a certain geography with a target of 3-5 assets in a market. We have a brand strategy. We will go anywhere in the U.S., in a primary or large secondary market. Imagine if Hilton told its regional directors that they were responsible to oversee all of its different brands. The operating models are so different. We are focused on executing successfully on singular brand strategies.
Mace: Isn’t scale important?
Kaplan: We have a strong, capable, committed team that can wear different hats. Our corporate director of frontline recruiting, for example, pitched in this week to fill a void at a property as sales director, assisting the team in day-to-day efforts. We have high performing talented people, and we sometimes pull them out to assist in other areas. That includes myself and our president, Jamie Ranzan. Our head of sales and marketing, Anna Wynn, even recently led our summit on memory care positioning. We have more corporate infrastructure than typical for a company of our size.
Mace: Where are your projects, and how many do you have?
Kaplan: We have eight properties. We operate in Florida, Virginia, Maryland, Illinois, Colorado, Texas, and Nevada. Most markets have one property. We’re looking to expand in Virginia and Maryland. That area, with its good demographics, fits with our brand strategy. We don’t go into commoditized markets that are price sensitive. We’re looking in places with certain home values, incomes, and net worths. We are also looking in upscale Florida markets. Broadly, we would not build in Florida. It’s too expensive to build given the market rents and care fees. But we can buy new vintage properties in the best markets if properties are priced appropriately to achieve a reasonable yield for our investors. Our growth strategy aligns with where we think we can outperform the broader market. We are a price leader. Our development deals are in the ultra-luxury segment. Some of the operators we respect that focus on similar markets and operational strategies are Belmont Village, Brightview Senior Living, and Kensington Senior Living
Mace: As a price leader, what can residents expect at Solera?
Kaplan: A great location, quality architectural design, and excellent services. Our buildings have a lot of natural light. We offer multiple dining venues, full service bars, beautiful outdoor spaces, wellness areas, fitness studios, and therapy gyms. Our residences are spacious and have high ceilings. In assisted living, for example, we feature full kitchens, balconies, and washers and dryers. Think of it as downsizing from a home but residents still have the amenities and features they are accustomed to. Our operational strategy is different too. All of our culinary directors are from restaurants, hotels or country clubs. We pay more for an executive chef. We spend more for food per resident, per day. We have more people working on the food line. We offer a large selection of made-to-order meals. Our staffing ratios are higher than the industry average, and we pay more for frontline workers and management. Our cost structure is higher too.
Mace: How would you generally characterize the acuity of your residents?
Kaplan: We have to provide more in the way of healthcare. We must have the clinical competencies that match the best of the best in the market. The company was launched as more of a social model, but the business has evolved. Our focus on a healthcare strategy is one of our biggest areas of change.
Mace: What is your healthcare strategy?
Kaplan: In 2020, I joined the board of EmpowerMe Wellness. At Solera, we contract with them for therapy services. They launched the integrated model which includes pharmacy and diagnostic services as well. EmpowerMe works with more than 1,000 senior living communities. We are also in the process of launching a program with a value-based primary care service provider, Curana Health. Curana includes a provider-led medical group, Medicare Advantage health plans, and a Medicare Accountable Care Organization. All senior living operators are going to need a value-based care strategy in the next 12 to 24 months. By partnering with a provider to coordinate care, the government saves money, and we can deliver a better experience for the resident. Senior living provides an important service and we should participate in the savings generated by value-based care programs. Most senior living operators, investors, developers, and advisors are not studying this yet.
Mace: How do you measure success?
Kaplan: Senior living is a juggling act to balance residents, families, team members, and investors. We continually assess how we deliver care and services. Are we attracting high performing team members and providing proper training? Are we meeting financial metrics for investors? Those are some of the key measures for me. We’ve operated through a pandemic, a staffing crisis, and the collapse of the capital markets. Now we are trying to restore margins while scaling thoughtfully.
Mace: What’s been the biggest surprise?
Kaplan: From an entrepreneur’s perspective, it’s how long everything takes. Building a high-quality operating company takes a long time. Development takes a long time. We started to underwrite our first deal, Kensington Maryland, in late 2016. We delivered the independent living portion in December of 2021 and assisted living in March 2022. You have to be comfortable being lean and hands-on in the early stages, and be prepared for everything to take a lot longer than expected.
Mace: Who are your capital partners?
Kaplan: We have three projects with AEW, two developments and a project they recapped. We’ve done three projects with Wheelock Street Capital and a programmatic venture with them for $300 million of equity. On the institutional side, we have a project with Berkshire Investment Group as well as several projects with family offices and high net worth partners.
Mace: What do you look for in a good capital partner? How have your capital partners responded to your needs during the pandemic?
Kaplan: Picking the right limited partner has been an important part of our strategy. I’ve seen what it’s like to work with 25 institutional partners. Some are short-term investors with a 1-3 year timeframe. Some are looking at demographics, trying to deploy a lot of capital and don’t understand the industry. Other groups don’t have good cultures and don’t value and respect their operating partners. AEW was the equity on our development in Kensington, Maryland. It gave me a great deal of confidence when the principals there said they would back me. Senior housing operations is tough. Having a partner who supports you during difficult times is better than getting a better share of the profits.
Mace: How is your current occupancy?
Kaplan: Our acquisition assets have a high 90% occupancy. Our first development deal opened in 2020 is in the high 90% range. Developments that were just opened in late 2021 are over 70% occupied. Those are big buildings and leasing ahead of projections. The Reserve at Lake Austin in Texas had 25 move-ins in the first 30 days and 28 in February. So, we have very good velocity. If you build or buy buildings that are well positioned, in good markets, and you have good operational leadership, the demand side of the equation is very strong from both an occupancy and revenue-per-occupied-unit perspective.
Mace: A lot of the stock of senior housing is more than 20 years old. In your view, can older inventory compete in today’s market?
Kaplan: Since 2016, the most important criteria we look for in an acquisition is the number of studios as a percentage of total units. Buildings with a significant number of studios under 400 square feet are difficult to lease and lease at a high enough rate per occupied unit to generate a fair margin and yield on investment. These projects may look good on paper, showing a low cost basis per unit, high margins, and really good overall returns. But we want to make sure we have something the consumer wants. Unit mix is number one. And I look for apartments of a certain size. We look for connection to the outdoors and a good amount of natural light in the building. How much space is dedicated to dining? We have full-service bars and have open kitchens. We have a casual dining area and a more formal area. Be mindful that residents are eating three meals a day every day in the community. We need to create spaces where they feel like they’re going someplace special. Wellness areas cannot be just a gym repurposed from an office space. Purpose-built therapy space is important. This plays into architectural relevance. You can buy new furniture and flooring and replace the lighting. But, if the bones of the building don’t support a design relevant for what the consumer is seeking today, those projects are obsolete and un-investable.
Mace: What about the need for middle market properties?
Kaplan: The middle market is a huge opportunity. The demographics are compelling. I wish I had a solution, but it’s difficult to see a viable middle market model in the near term. We need some type of government subsidy for a portion of the services we provide or a meaningful contribution from value-based health care program. Or we need significant advances in technology to operate more efficiently. I’m optimistic about advancements in technology and the use of artificial intelligence in particular could realize efficiencies. We see more entrepreneurs coming in to solve problems around aging and healthcare. I’m optimistic about innovations that will improve operations.
Mace: Our readership includes younger professionals starting off in their careers. What advice can you provide to them?
Kaplan: It’s good for someone early in their career to forecast where they want to go, and work backwards. What do you need to learn to get where you want to be? Early on, they might look for the most money. But I think it’s better to consider where they will get the best mentorship and experience, and prioritize that over compensation. I am a big proponent of learning operations. There is a shortage of young talented operators.
Mace: Lastly, is there anything else you would like our readership to know?
Kaplan: I’d like to see more collaboration among industry thought leaders to address our sector’s structural problems and to create a sustainable business model. The demand side is good if you have a well-positioned property. But margin compression is real. Also, I am a big proponent of immigration reform. We need smart immigration policy. We need to bring people into this country to work front line healthcare jobs. This has to be a priority for anyone focused on policy in this industry.
Are Seniors Better Together? The Effect of Housing Status on Excess Mortality During COVID-19
by Ryan Brooks, Senior Principal, NIC
The COVID-19 pandemic has been devastating for older adults in the U.S., particularly those with existing chronic medical conditions and complex health care needs. Many of the individuals most impacted by COVID-19 reside in nursing homes, a setting that accounted for at least 25% of all COVID-19 deaths. This setting is often conflated with senior housing, even though they are distinct care settings and serve different, although at times overlapping, populations.
To maintain the health and safety of residents, improve infection control procedures, and navigate potential future pandemics, it is imperative that there be an understanding of the impact that seniors’ housing type had on excess mortality—the difference in mortality rates during the pandemic relative to deaths before the pandemic. In order to garner this improved understanding, NORC at the University of Chicago, on behalf of NIC, conducted a landmark study comparing excess death rates for older adults living in senior housing, long-stay nursing homes, and non-congregate residential settings in the community at large.
The study – ‘The Effect of Housing Status on Excess Mortality During COVID-19’ – builds upon research previously conducted by NORC on behalf of NIC. Findings from earlier stages of the study concluded that COVID-19 mortality rates across seniors housing increased as the health and caregiving complexity of residents increased, with the highest percentages occurring in memory care settings and skilled nursing properties. Memory care units faced particular challenges with infection control, since seniors who have cognitive impairments are more likely to require additional care and support for basic needs.
The second and final phase of the study measured excess death rates for older adults by housing and care setting across two distinct time periods – one prior to vaccine availability and another post-vaccine availability. The study also took into consideration the health status, demographic characteristics, health care usage, and geographic location of older adults to allow comparisons of comparable older adults regardless of where they lived. This methodology improved upon findings from earlier phases by risk-adjusting for age and health status.
Prior to vaccine distribution, older adults living in congregate senior living and nursing care settings did have greater excess mortality than those living in residential non-congregate settings in the community at large. Given what we now know about COVID-19 transmission, the inherent risk for those with underlying health conditions, and the elevated risk for persons who require close contact caregiving, this is an expected finding.
Study results for the post-vaccine implementation period, however, highlight how excess mortality in senior housing settings fell to similar rates as the non-congregate settings. A possible explanation for these findings is that vaccine availability, distribution, and uptake among residents in congregate settings led to earlier vaccination and ultimately improved outcomes. Senior housing and nursing home settings were among the first to receive vaccines and conduct on-site vaccine clinics for residents and staff. Earlier vaccine rollout may have led to a return to socializing for the independent living cohort or stress reduction amongst those receiving vaccines. Thus, earlier vaccine administration may have had a protective impact on certain risk factors, such as isolation and loneliness.
A possible explanation for these findings is that vaccine availability, distribution, and uptake among residents in congregate settings led to earlier vaccination and ultimately improved outcomes. Senior housing and nursing home settings were among the first to receive vaccines and conduct on-site vaccine clinics for residents and staff. Earlier vaccine rollout may have led to a return to socializing for the independent living cohort or stress reduction amongst those receiving vaccines. Thus, earlier vaccine administration may have had a protective impact on certain risk factors, such as isolation and loneliness.
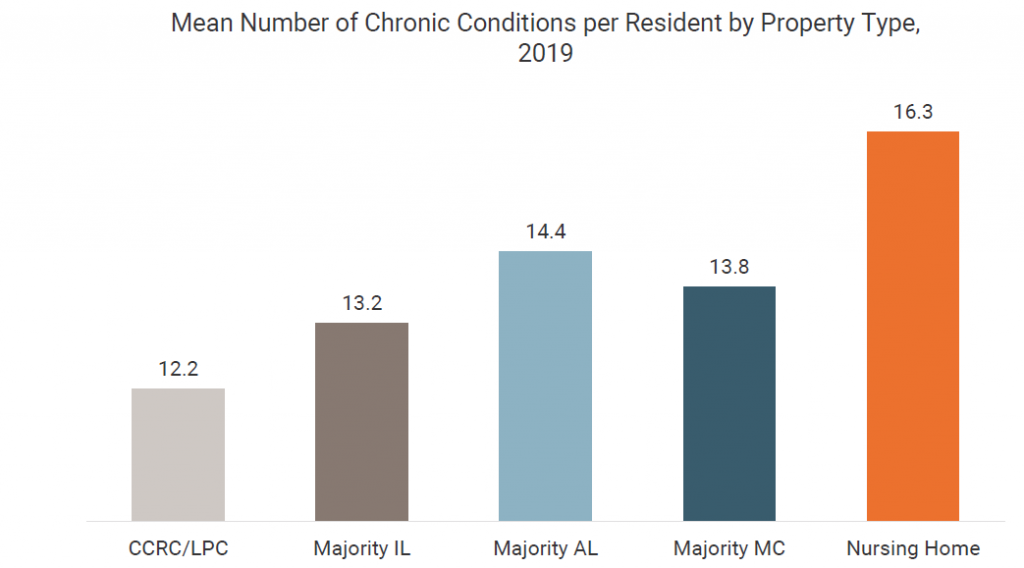
One of the study’s key conclusions emphasizes how long-stay nursing care differs from senior housing regardless of vaccine availability. In both the pre-vaccine and post-vaccine study periods, long-stay nursing homes had a greater rate of excess mortality than senior housing. Study findings related to the number of chronic conditions residents have by property type underscore a key contributing factor: residents in a skilled nursing setting average more than 16 chronic conditions.
While residents in other senior housing settings also have a significant number of chronic conditions, it is residents of skilled nursing who are at the top. This conclusion is consistent with findings from Phase I of study that show COVID-19 mortality rates increase as the health needs and caregiving complexity of residents intensify.
The study introduced a new way to use Medicare claims data to assess the health and outcomes of older adults in senior housing and nursing care settings compared with the community at large. The methodology for the study utilizes an academically-designed data linkage approach which combines property information from NIC MAP® Data Service, powered by NIC MAP Vision, with Medicare claims and administrative data. The analysis allows for comparisons of comparable seniors across disparate living settings and is among the first to utilize an accurate, extensive list of senior housing properties matched to Medicare administrative data to identify residents of seniors housing, nursing homes, and non-congregate settings.
The connection between housing and health is a critical one; importantly, this study demonstrates the feasibility of utilizing administrative claims data and property data to advance the understanding of the health and outcomes of older adults residing in senior housing settings.
View the complete white paper and associated slide deck of findings, including methodology, inclusion criteria, results, and conclusions, on our website.
Exploring the Interplay Between Inflation, Rate Growth, Demand and Occupancy in Senior Housing : An In-Depth Analysis of NIC MAP Vision Actual Rates Data
by Beth Mace, Chief Economist and Omar Zahraoui, Principal
The following is an excerpt of the NIC Notes blog article under this same title. To read the entire in-depth analysis, please visit NIC Notes.
Executive Summary
Through this in-depth analysis, we hope to shine a spotlight on the relationship between inflation, the pace of growth seen in-place actual rates, demand and occupancy. Actual in-place rates refer to effective rates or the rates that are “actually being paid” to live in senior housing. This is often not the same as the asking or listing rate that may be advertised or listed in a brochure.
NIC MAP Vision Actual Rates data has been collected for the last eight years with the ongoing aim of NIC to bring greater transparency into the industry. More specifically, this effort has included the collection of rent roll metrics on move-in, in-place and asking rates.
The full article is separated into three sections:
- Section 1 provides background on the data collection process and its importance as well as the evolution of the actual rates database.
- Section 2 looks at the relationship of inflation to in-place rate growth since the onset of the pandemic by specific senior housing care segments, i.e., independent living, assisted living and memory care, and finds distinct patterns of rate growth based on the level of inflation.
- Section 3 takes a deep dive into actual rates data to uncover property level insights on the pattern of rate growth, occupancy and demand. Notably, this is one of the first in-depth analyses conducted on this data since the launch of the Actual Rates Data Initiative by NIC MAP Vision in 2015. This analysis was conducted using quintiles to examine the distribution of in-place rate growth in December 2022 from year-earlier levels on a same store basis.
We start with a summary of key findings.
Unveiling the Key Takeaways
Having good data processes in place can be considered as a proxy for better management and performance when evaluating a senior housing property, as well as an indicator of how the sector is evolving on a broader scale.
The year-over-year pace of growth in in-place rates for all care segments generally stayed moderate and largely aligned with the inflation rate in 2020. However, in the first half of 2022, as inflation reached 40-year highs, senior housing in-place actual rates also rose to record highs from year-earlier levels across all senior housing care segments despite the market’s still relatively low occupancy levels in general.
A notable relationship exists between in-place rate increases, demand growth and the pace of occupancy recovery. These relationships differ between independent living care segments (frequently more of a lifestyle choice than need-driven) and assisted living care segments/memory care segments (more of a need-driven than lifestyle choice).
For the independent living care segments (frequently more of a lifestyle choice than need-driven) the data shows that the stronger the demand, the greater the pace of increases in in-place rates. Notably, annual increases in in-place rates are highly associated with stronger demand and improvements in occupancy rates.
The relationship is NOT the same for the assisted living care segments and memory care segments – (more need-driven than lifestyle driven). For these segments, the data suggest that there is negative correlation between in-place rate increases and demand growth/occupancy recovery. This means that, as year-over-year in-place rate increases get smaller, there is a stronger demand growth and occupancy recovery, on average.
Additionally, there is evidence that operators bought occupancy by limiting rent growth. That is, the lowest occupied assisted living and memory care segments were able to generate new demand and grow occupancy faster, but this occurred largely because of minimal or even negative rent growth. And on the other hand, the highest priced assisted living and memory care segments were able to command the most rate growth, maintained relatively stable occupancy, but saw little net new demand.
Further, the analysis also highlighted the importance of understanding what current and potential senior housing residents are willing to pay and the potential impact of higher rate increases on the pace of move-ins and move-outs, demand growth, and occupancy recovery—as it pertains to in-place rates.
Section 1– Good Data, Good Management: The Link Between Effective Data Processes and Performance.
“With data collection, ‘the sooner the better’ is always the best answer.” — Marissa Mayer
Data powers everything that we do. We live in a data-driven world, which means, without accurate, relevant, and timely data, it is nearly impossible to make informed decisions, evaluate risks and opportunities, understand the context in which we operate, and develop effective business solutions in today’s constantly evolving markets.
For the senior housing and care sectors, collecting and applying accurate data is as important as ever. That said, it is fair to acknowledge that it is not always an easy task for many senior housing and care providers. Data collection involves both human and technological resources, including well-designed organization structure, data collection and storage infrastructures, and efficient internal processes. Having good data processes in place can be considered a proxy for better management and performance when evaluating a senior housing property, as well as an indicator of how the sector is evolving on a broader scale.
The Evolution of NIC MAP Vision Actual Rates Data: Is the Senior Housing Sector Meeting the Needs of Today’s Market?
One of the many strategic initiatives undertaken by NIC and NIC MAP Vision over the years has been the NIC MAP Vision Actual Rates Data Initiative. This has been driven by the need to increase transparency in the senior housing sector to achieve greater parity to data that is available in other real estate property types.
This strategic initiative provides accurate data on the monthly rates that senior housing residents are specifically paying compared to properties’ asking or listed rates. The dataset includes nearly eight years of data for in-place rates, move-in rates, asking rates, occupancy, and leasing activity, as measured by monthly move-in and move-out velocities from April 2015 through December 2022.
Each quarter, NIC MAP Vision releases monthly time series of actual rates comprised of end-of-month data for each respective month. The release includes aggregate national data across senior housing property types (i.e., majority independent living and majority assisted living) and senior housing care segments (i.e., independent living, assisted living, and memory care).
In recent years, the dataset has grown to report the aggregate data for select metropolitan markets at the care segment level (12 markets for the independent living care segment, 22 markets for the assisted living care segment, and 16 markets for the memory care segment) to gain a comprehensive understanding of markets and their actual rates dynamics. This data collection has provided the ability to compare move-in and move-out velocity measures and, importantly, an assessment of discounts and concessions being offered to residents as they move into properties. However, reporting additional markets relies upon participation rates of the individual market’s senior housing operators.
Participation from all senior housing providers is key to increasing transparency in the sector and meeting the needs of today’s market. The more accurate data that is collected, the more reliable the conclusions and valuable the insights will be. This not only benefits the industry as a whole, but also individual operators who can use the insights gained from analyzing actual rates data for improved decision making and better outcomes for all stakeholders involved.
To read the insights from the blog’s remaining Sections 2 and 3, which include the first-ever analysis at the property level of the distribution of senior housing in-place rate growth across all senior housing care segments, please visit the NIC Notes blog.
Interested in learning more?
To learn more about NIC MAP® data, powered by NIC MAP Vision, and accessing the actual rates data, schedule a meeting with a product expert today.
NIC MAP Vision welcomes your participation by contributing your properties’ data to the actual rates data set. To find out more, visit NIC MAP Vision.
Innovations in AgeTech at the 2023 Consumer Electronics Show
by Ryan Brooks, Senior Principal, NIC
The annual Consumer Electronics Show (CES) convenes each year in Las Vegas and brings together some of the world’s best tech companies to showcase their latest advancements. Highlighting the importance of technology and longevity at CES is the AgeTech Collaborative, which showcases digital technologies that are built around the needs and wants of older adults, often with their explicit input during the design process.
With major increases in tech adoption by older adults, as well as their care providers, the AgeTech market is expected to grow to $2 trillion in the coming years. AgeTech is more than simply making devices with larger buttons, brighter screens, and bigger text, however. While adapting existing technology to make it easier for seniors to use is both welcomed and useful, true AgeTech goes beyond that by incorporating the ultimate end users of the product into an integral step in the design process, allowing for an end result that is much more appropriately suited to their needs.
While many of us may be familiar with the most common AgeTech on the market, such as wearable technology for tracking vital signs, the Consumer Electronics Show offers up breakthrough technologies that hope to aid older adults to live happy, healthy, and meaningful lives. In fact, there is so much attention being paid to AgeTech that a specific AgeTech Summit was launched at this year’s CES. The Summit consisted of a dedicated program of key speakers and panel discussions all focused on the space.
Below are some technological highlights representing the AgeTech space from the 2023 Consumer Electronics Show. Each technological advancement below is organized according to the key domain area in which it is positioned – smart home, digital health, social engagement, or accessibility.
Smart Home | ZIBRIO – The Balance Company
Addressing balance and fall issues is a high priority in any senior living community. ZIBRIO provides measurement-based fall prevention along the continuum of care. With a brief 60-second test, residents can be stratified into high, medium, and low-risk categories. ZIBRIO’s Stability Pro scale provides a balance score that predicts if an older adult will fall in the next 12 months, and accompanying software guides the physician or care team with personalized recommendations and care.
The ability to easily conduct a fall risk assessment for residents can add substantial value to senior living communities. The short time it takes to conduct the assessment means that these important proactive steps to fall prevention can more routinely be conducted. No longer will fall risk assessments be limited to once or twice per year. Additionally, the ZIBRIO approach works hand in hand with existing systems and specialist personnel, like physical therapists and fitness instructors who may already be working with your residents.
Digital Health | Flowly – Master Your Nervous System
In response to the increasing behavioral health challenges being identified among the senior population, Flowly has developed a platform for people with chronic pain, anxiety, and insomnia who are seeking to take control of their health. Flowly is a mobile application that combines virtual reality and biofeedback training to teach a user how to reclaim their body and mind each day. The virtual reality headset is worn in the comfort of one’s own residence and is designed to bring relaxation and comfort.
A key goal of Flowly is to teach the user how to better control their nervous system. A sensor in the Flowly kit collects real-time heart rate information that is shared back to the user. Breathing exercises and guided sessions teach the user how to become more aware of their body, their mind, and ultimately their needs. The platform even allows users to meet and connect with like-minded people to form support groups, in-person events, and community forums.
Social Engagement | Beeyonder, Inc.
Beeyonder is a customer centric virtual tour company whose mission is to create opportunities for older adults to explore the world from the comfort of their own residence. The Beeyonder experience includes qualified and local guides that will take users on a remarkable adventure, provide captivating stories, break down social barriers, and invite users to experience new cultures.
Beeyonder offers a ‘Passport Club’ that can be acquired for an individual, a group, or even purchased for a corporate account. Subscription packages offer flexibility with regards to the number of tours organized – there are monthly, three-tour, six-tour, or 12-tour subscription options. Groups can take one tour per month or use the multi-tour options to take tours throughout the year or take more than one tour in a month.
Accessibility | RAZ Mobility
RAZ Mobility developed and sells the RAZ Memory cell phone – an easy-to-use groundbreaking cell phone for people with dementia, stroke, Parkinson’s disease, low vision, general cognitive decline, or even for seniors who may generally be tech-adverse. What makes the RAZ cell phone special is a Remote Manage feature that provides caregivers an unprecedented ability to remotely control aspects of the phone remotely through a simple application or online portal.
The RAZ cell phone is relentless in its focus on simplicity. The phone consists of a single primary screen, with three elements:
- Pictures and names of up to six contacts (with the option to increase to 30)
- A button to call 911 (or alternative RAZ emergency service)
- Time and battery power
There are no applications or settings that may cause confusion to a user. There are no notifications or operations system updates to manage. The user simply taps the picture of the person they wish to call, and they will be connected. While not always the case with technological advancements, in this case, the value really is in the simplicity of the offering.
In summary, as evidenced by the sheer number of featured startup companies highlighted at the AgeTech Collaborative at the 2023 Consumer Electronics Show, there are tremendous advancements being made in the effort to improve people’s lives as they age. It behooves senior housing and care operators to be aware of the latest technological advancements being made in the AgeTech space, as many of these products and services will improve the day-to-day lives of their residents, ease the ongoing staffing challenges, and ultimately differentiate their communities.
“No-Regrets” Moves to Make Today with Your Healthcare Provider Partners
by Kyle Gardner, COO, NIC MAP Vision
 Our industry is experiencing renewed focus on the partnership between senior housing communities and the healthcare providers who care for their residents. With a shared mission of resident health and wellness, housing and care partners are weighing emerging options to align incentives and integrate operations. At NIC MAP Vision, we have a unique vantage point on the connection between senior housing operators and healthcare providers – we serve both groups, so we gain perspective on both sides of the partnership table, and how it might change in coming years. New care delivery models and new payment models are capturing headlines, and both housing and care providers are working to define their future strategy. We wanted to share some “no-regrets” steps that senior housing operators can take this year to strengthen their relationships with their providers and provide a flexible foundation for many potential future tactics.
Our industry is experiencing renewed focus on the partnership between senior housing communities and the healthcare providers who care for their residents. With a shared mission of resident health and wellness, housing and care partners are weighing emerging options to align incentives and integrate operations. At NIC MAP Vision, we have a unique vantage point on the connection between senior housing operators and healthcare providers – we serve both groups, so we gain perspective on both sides of the partnership table, and how it might change in coming years. New care delivery models and new payment models are capturing headlines, and both housing and care providers are working to define their future strategy. We wanted to share some “no-regrets” steps that senior housing operators can take this year to strengthen their relationships with their providers and provide a flexible foundation for many potential future tactics.
Each senior housing organization will develop their own approach in the next one to two years that fits their goals for resident health, operating and financial conditions, and appetite for risk and innovation. One thing is for certain amid a diversity of approaches – no organization can optimize resident health alone. Senior housing communities and healthcare providers will need to navigate a changing care landscape together.
In the meantime, provision of healthcare to senior housing residents remains a desirable line of business for providers. Our data at NIC MAP Vision shows continued consolidation of healthcare spend within senior housing buildings to single providers in key service lines like hospice, home health, and primary care. Providers are “pairing off” with senior housing operators across the market, and they are motivated to craft unique value propositions for their strategic senior housing partners. Providers are becoming more-savvy at partnership with senior housing communities that fit their business the best – for example, primary care groups who receive reimbursement for attributed ACO beneficiaries are seeking geographic concentration. Hospice agencies seek senior housing communities with the right mix of residential settings to support the length of stay that supports their margins.
Both healthcare providers and senior housing operators are trying to join together in robust and productive ways based on today’s business conditions.
We believe there are steps that senior housing communities can take right now that form a “no-regrets” foundation to prepare for industry shifts in the provision of healthcare. Here are the four tactics that senior housing owners or operators should do today:
- Map your healthcare stakeholders
- Define the metrics that matter for your residents
- Know who provides care in your market
- Define your decisionmakers
1) Map your healthcare stakeholders
Who provides care to your residents today? You may know the major players, like the long-term care pharmacy you contract with, or the hospice providers you work hand-in-hand with. We believe that each senior housing operator should know the top providers by reimbursement for their residents in the following ancillary services:
- Pharmacy (both long-term care and retail)
- Primary care
- Rehabilitation services
- Hospice
- Home health
- ACO attribution
Knowing all of the key healthcare providers in your community highlights opportunities to forge partnerships that align with your future strategy, either by deepening a relationship to a trusted incumbent provider or by exploring other potential partners.
2) Define the healthcare metrics that matter for your residents
Comparative data will be a keystone of any industry-wide shift to value-based payment, and no matter how you choose to engage with novel payments, you’ll be asked to operate effectively in a more data-rich environment. Today, senior housing operators are uneven and sometimes reactive in the way that they hold ancillary healthcare provider partners to a performance standard – we have heard “we take a closer look at the KPIs after we hit some bumps in the road.” We suggest that senior housing operators refresh their ability to evaluate new providers’ quantified performance and to hold existing partners to clear standards. Senior housing operators know to rely on public quality data when vetting providers, but we expect more of them to set and track their own criteria in addition.
3) Know who provides care in your market
Don’t overlook great potential partners in your own backyard, and stay current on what a best-in-class partnership might offer you. NIC MAP Vision has invested in a data tool, scheduled for launch later in 2023, that will allow senior housing operators to browse providers by geographic market, and see highlights of their unique service offerings. We believe that senior housing operators shouldn’t rely solely on outreach from prospective provider partners – the healthcare services they provide are too essential for residents’ wellbeing. Seek out provider partners when you need them with a comprehensive and proactive scan of the market.
4) Define your decisionmakers
Which leaders inside your organization make decisions about healthcare provider partnerships? Is this decision structure the same for all ancillary services? For all regions or communities? Don’t be shy about directing prospective healthcare partners. Share the right way and the right time to approach your specific decisionmakers and any decision criteria they use. For larger organizations, a formal RFP process may be the best way to establish healthcare partnerships. Smaller organizations may not need the full structure of an RFP but can still benefit from internal stakeholder agreement on key criteria. Even without a full-blown RFP process, you can provide elements of guidance to providers by defining and sharing your decision criteria, focusing productive conversations on your organizational goals.
The senior housing and care ecosystem is poised for change, but these four steps will clarify your current status in each ancillary service and give you a foundation to work from as you plan your next strategic arc. Your portfolio of healthcare provider relationships is complex even in advance of any aligned incentive structures, so keep each step current as connections shift with normal market dynamics.
Finally, as you weather industry-wide shifts, don’t forget that your healthcare provider partners impact your residents’ wellbeing, their families’ experiences, and your own staff’s workflow and capacity. Alignment with your mission and standards of care can always be centered among your partnership criteria. The best healthcare providers bring your mission to life with the operational realities of bedside care and fit your community culture like an extension of your own staff. The best partnerships bring senior housing and care together seamlessly around each resident and enable all parties to sustain their commitment to serving the community.