How Could the Proposed Senate Health Care Bill Impact the Nursing Home Sector?
In March, when the Republicans in the House submitted a proposal to repeal and replace the Affordable Care Act (ACA), this Blog series provided a brief overview of how the proposal could affect the skilled nursing sector. Now that the Republicans in the Senate have released their own proposal, it’s again time to briefly review the key points of the legislation that could have an impact on this sector. Some differences exist between the two versions of the bill, but for this discussion, one of the key points is that both propose significant cuts to Medicaid, which funds the majority of nursing home residents’ care.
Keep in Mind that Governance Is a Process
The Better Care Reconciliation Act (BCRA) is the Senate’s response to the American Health Care Act (AHCA), which passed the House earlier this year. The Senate was not able to hold a vote on the BCRA prior to recessing for the Independence Day Holiday, due in part to the Congressional Budget Office’s (CBO) estimate that 22 million Americans would become uninsured by 2026 as a result of the bill. When the Senate comes back from recess in the second week of July, it will likely adjust the BCRA to try and get passage of the bill. To date at least nine Senators have pledged to not vote for the BCRA in its current state; for the bill to pass, the vote needs 50 of the 52 Republican Senators to agree upon the legislation.
In terms of process, the rewrite could be quick, drawn out, or a not even happen. If the dissenting Republican Senators can be assuaged easily with minor adjustments (not likely given the degree of disagreement), then a new version of the bill could be quickly put to a vote after some debate and a new analysis from the CBO. On the other hand, if the adjustments needed to satisfy Sens. Rand Paul (R-KY), Susan Collins (R-ME), and others require lengthy negotiations (or even a return to the drawing board altogether), several weeks could be dedicated to the rewrite before the bill goes back to the CBO, gets debated on the Senate floor, and then goes to a vote. Senate Majority Leader Mitch McConnell is only likely to call for a vote on the BCRA if enough Republican Senators pledge to pass it. If the BCRA passes, it will then go through the reconciliation process, which is where the House and Senate versions of the bill become reconciled, and which will be a challenging exercise given the controversy over the bills.
Here’s What Critics Are Saying about the Impact on Nursing Homes
Sen. Al Franken (D-MN) on CNN’s “The Lead“: “This is a terrible bill” because “it cuts Medicaid to the same degree that the House bill does. It just delays it some, and it’s hundreds of billions of dollars from Medicaid, which helps kids, the disabled, seniors. Sixty percent of seniors get their nursing home care from Medicaid. And all of that money that’s cut from Medicaid pays for a huge tax cut for people who are doing very well.”
Mark Parkinson, President and CEO of the American Health Care Association, in reference to the provision changing how the growth rate in federal matching dollars for Medicaid is calculated and decreasing allowable provider assessment that determines federal matching dollars tied to provider revenue: “If these provisions stay in the legislation, the long-term impact of these will be debilitating to the sector and to the people that rely on long term care.” (Provider Magazine)
AARP, in a press release, “In terms of seniors, we have serious concerns about setting caps at a time when per-beneficiary spending for poor seniors is likely to increase in future years. By 2026, when Boomers start to turn age 80 and older, they will likely need much higher levels of service — including home and community-based services (HCBS) and/or nursing home care — moving them into the highest cost group of all seniors.”
The Bottom Line Hasn’t Changed – Medicaid is Still Critical to Nursing Homes
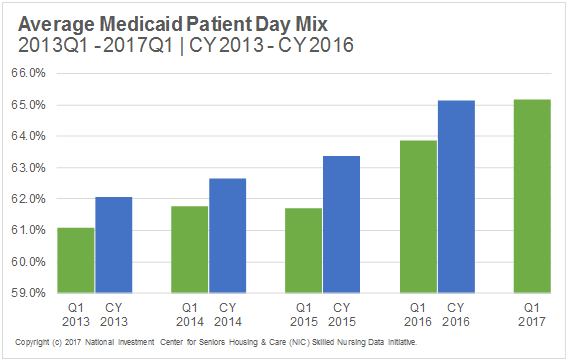
As we said when the AHCA proposal came out of the House, any changes to the Medicaid program will have an impact on the nation’s nursing homes. Per the most recent Skilled Nursing Data Report, which includes data going back five years and is as recent as the end of Q1 2017, Medicaid is the main driver behind occupancy of nursing homes. Indeed, 65.2% of patient days at the end of March 2017 were attributed to the Medicaid program (referred to as Medicaid patient day mix). Medicaid patient day mix has been growing over the last five years, due in part to Medicare initiatives to drive down utilization of skilled nursing for post-acute care. In fact, if the pattern from the last four years continues, with Q1 Medicaid patient day mix tending to be lower than the average for the calendar year, we might expect that the average Medicaid patient day mix for 2017 will reflect the same growth pattern. Any policy that carries a major impact on the states’ Medicaid budgets will result in an impact on nursing homes.
The Home-and-Community-Based Services Question
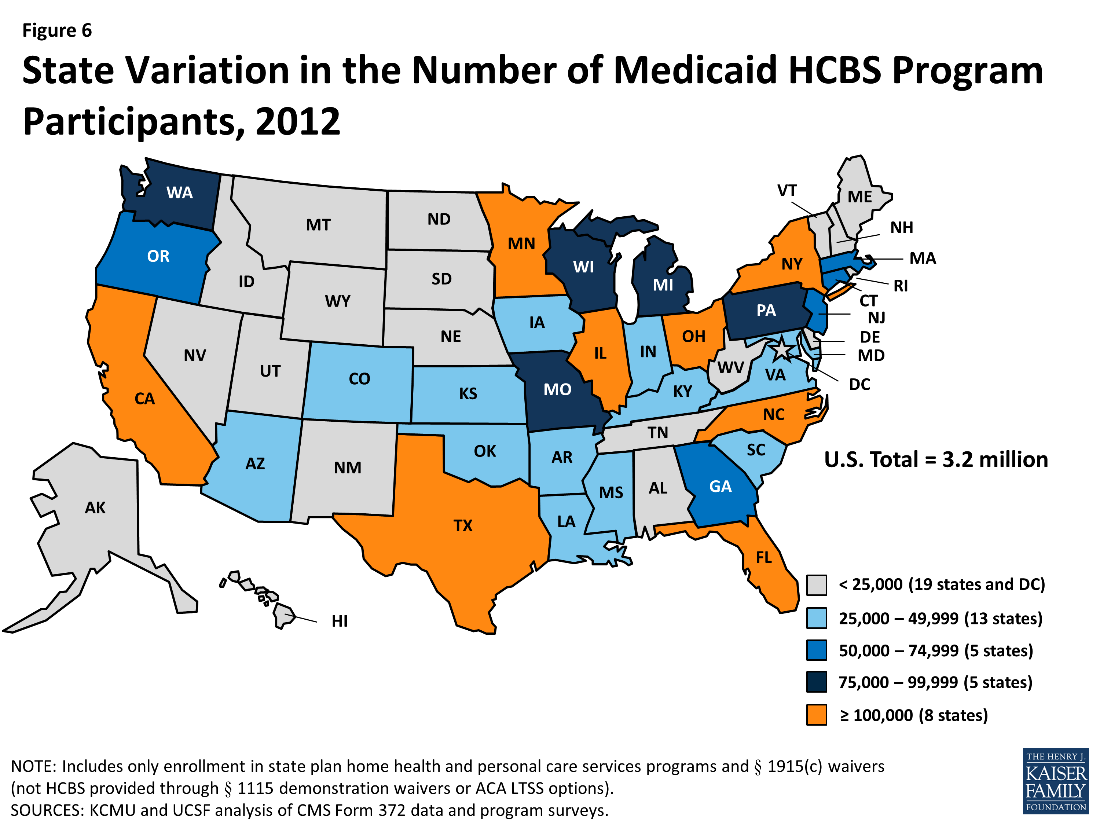
While many (see above) have voiced their opposition to the Senate’s bill because of its impact on nursing home residents and seniors, two provisions of the proposal has some potential to give a boost to the sector. The first boost may come as a result of elimination of the employer mandate to provide health insurance; removing this requirement may give providers an opportunity to reduce their overall cost of operations. The second provision that could increase nursing home utilization among Medicaid beneficiaries is the elimination of an incentive payment instituted by the Affordable Care Act under the Community First Choice program, which encourages states to use home-and-community-based services (HCBS) instead of institutional care (see page 33 of the CBO report). The premise behind the Community First Choice program is that HCBS are an inexpensive way to provide the types of care one would otherwise receive in a nursing home, a service delivery alternative that could become increasingly attractive to states facing shrinking Medicaid budgets as a result of healthcare reform. This program and other waivers under Medicaid for HCBS are considered optional, which is why some have said the Senate Bill will reduce HCBS spending. An important distinction, however, is that HCBS spending is an optional alternative to nursing home care for people who are on Medicaid and nursing home-eligible. Medicaid-funded care for that population is not optional, the setting of care delivery is. Indeed, HCBS spending has grown considerably in the last 20 years, but the Community First Choice waiver specifically has not been widely popular, with only a few states opting into the program. The map below shows participation in any HCBS program in 2012, including Community First Choice participation.
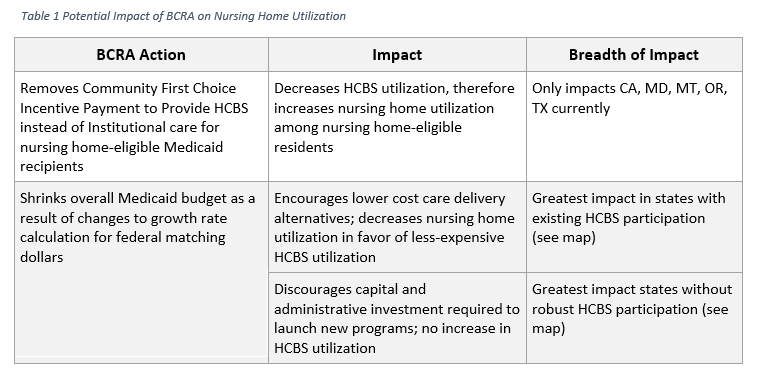
A GAO report found that many of the barriers to entry into the program cited by states that had not submitted applications for the waiver (and thus forwent the bonus payment incentive) were associated with administrative costs. So, while the bill removes an incentive to spend more on HCBS, which could increase nursing home utilization, tighter overall Medicaid budgets would encourage states to opt for less expensive service delivery options, pushing residents into HCBS instead of nursing homes. The administrative burden of establishing HCBS could further disincentive states from taking advantage of the program because of the immediate impact on the budget, especially in states that do not already have robust HCBS program participation.
For now, we wait for the process to play out. If lawmakers remain intent on repeal-and-replace and reforming Medicaid simultaneously, as is the course both houses of Congress have followed up to this point, then we may anticipate considerable changes to the Senate legislation before a “passable” version of the bill is produced. In the meantime, senior advocates will be lobbying Washington, op-eds in favor and against the legislation will be printed in newspapers, and NIC will continue collecting data.